Sleep is our body’s wonder magic to keep it healthy and maintain several physiological functions balanced. Studies say that an average person spends one-third of his entire life in sleeping. But, one in every five individual suffers from sleep-related disorders; yet sleep issues are often ignored, under-diagnosed and inadequately treated. While central sleep apnea usually occurs in association with heart failure, the ascent to high altitudes and usage of opioid medicines, common risk factors for obstructive sleep apnea include – obesity and abnormal anatomy of the upper airway resulting in airway crowding.
What is sleep apnea?
It is a disorder wherein there are frequent interruptions in one’s breathing during sleep. This may be in the form of significant airflow limitation during breathing while a person is asleep or complete cessation of breathing during sleep. Together they are known as “Sleep-related breathing disorders”.
For an average individual, upto five such interruptions are considered common. But when this number goes to fifteen, the brain and the rest of the body does not get sufficient oxygen. Because of the non-specific nature of the symptoms, patients usually remain undiagnosed until they suffer from long-term consequences of the disorder. According to a study featured in the ‘American Journal of Critical Care and Respiratory Health’, untreated sleep apnea is not only associated with increased risk of heart and brain disorders but also associated with increased mortality, thus earning the name of ‘silent killer’ for this disorder.
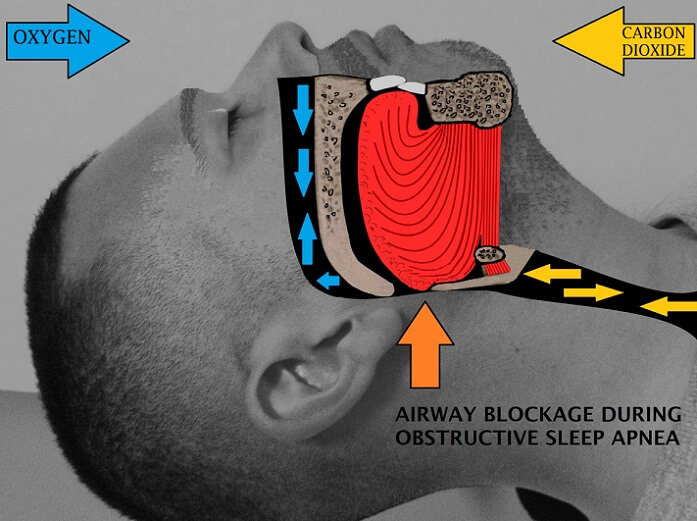
Symptoms of sleep apnea:
The common symptoms of sleep apnea are:
- Loud snoring
- Excessive daytime sleepiness
- Non-restorative sleep
- Difficulty falling asleep
- Morning headaches
- Dry mouth in the morning
- Choking during sleep
- Breathing pauses witnessed by bed partner during sleep
Consequences of sleep apnea:
If untreated, a sleep apnea patient may experience the following consequences gradually.
- Impaired concentration and memory resulting in impaired work performance and easy fatiguability
- Increased risk of vehicle and workplace accidents
- Irritability and mood swings
- Impotence and depression
- Drug-resistant hypertension, heart attack and cardiac rhythm disturbances
- Stroke
- Increased risk of diabetes and liver disorder
How to diagnose sleep apnea?
The analysis is based on a combination of clinical features and subjecting the patient to investigations. There are particular questionnaires to assess a person’s tendency to excessive daytime sleepiness (Epworth sleepiness scale) and his or her risk of developing sleep apnea (Obstructive Sleep apnea). In patients with symptoms suggestive of a sleep-related breathing disorder and associated risk factors as outlined above subjecting them to overnight sleep study confirm the diagnosis.
‘Polysomnography’ or sleep study remains the gold standard for the diagnosis of sleep apnoea. Ideally, to be conducted under supervision in a hospital setting, it assesses the patient’s airflow, snoring, brain activity, breathing patterns, oxygen levels and body & leg movements while the patient remains asleep. In certain situations, it can also be conducted at home without supervision but has limitations of assessing fewer parameters and can only be used to screen at-risk patients.
Treatments:
Conservative measures:
- Medical treatment of nasal congestion – Decongestants
- Stop Alcohol & smoking
- Positional therapy
- Considered in whom sleep apnea is more common in the supine position
- Treatment consist of using special pillows or other positioning devices to help them avoid supine sleep
Oral appliances:
- Designed to keep the upper airway patent during sleep
- Various types such as Tongue retaining device and Mandibular repositioning device
Surgical treatment:
- The surgical candidacy of the patient is determined after a thorough evaluation in select cases
- Most commonly performed surgery is ‘Uvulopalatopharyngoplasty’.




![The Top & Most Popular Seafood Bucket Restaurants in Dubai for you [Never Miss]](https://uae24x7.com/wp-content/uploads/2020/09/8-seafood-in-a-bucket-scaled-e1600739237403.jpg)
![Procedures for Renewing the Driving License in Abu Dhabi [3 Simple Steps]](https://uae24x7.com/wp-content/uploads/2020/07/Capture-9-e1595666454466.jpg)





