At least a dozen companies have come up with Covid-19 vaccines, which they claim, are more than 90 per cent effective. While it is cock sure that the whole world population cannot be immunized at once, serious discussions are going on about what category of population should be inoculated first.
Some advocate that the elderly and more vulnerable need to be given priority. But many oppose this by arguing that those categories are not that much socially interactive and hence the young should be vaccinated first, as they are more socially active.
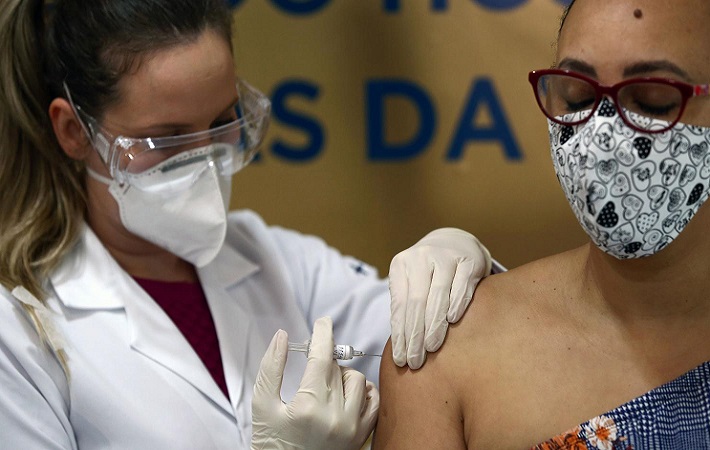
Some nations, such as the UK, are prioritizing primarily by age, in line with the pattern that mortality rates increase steeply as people get older. Greatest priority is given to older adults in care homes and care home workers, followed by those over 80 and healthcare and social care workers. It is only when all over-65s have been offered the vaccine that high-risk adults younger than 65 will be included, which could be mid-2021 or later.
According to David Taylor, professor emeritus of pharmaceutical and public health policy at University College London, it is “a sensible way forward” to focus on those at raised risk who can safely be given a vaccine.
“The easiest way to do that is by age. I think it’s a reasonable strategy,” he said. While there are detail differences among other major European countries, such as Germany, Italy and Spain, they too are also focusing on those most vulnerable because of health conditions or age, plus healthcare workers.
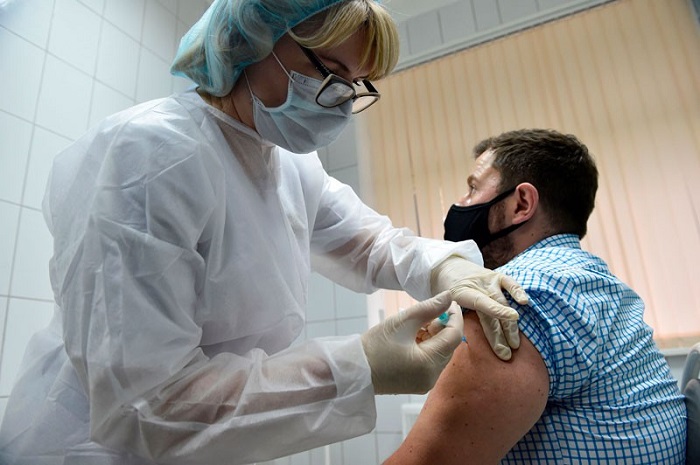
France’s approach is similar but casts a wider net when it comes to people at increased risk because of their occupation. Their prioritized list includes 23 million people who are elderly or have underlying medical conditions, plus 1.8 million workers in healthcare and related sectors, and 5 million taxi drivers, shop workers, school employees and others who have frequent contact with the public. Taxi drivers are reported to have suffered high mortality early on in the pandemic.
The US Centre for Disease Control (CDC) suggests that, along with other at-risk groups, members of ethnic minority communities could be prioritized because they have been hit harder by the virus.
Latest research from Khalifa University, however, appears to upend conventional wisdom when it comes to whom vaccination programmes should focus on.

Computer modelling suggests priority should be given to people who have most interactions with others, typically younger individuals, even if they themselves are unlikely to fall seriously ill should they contract the coronavirus.
Under one scenario modelled by the researchers (involving 75 per cent vaccine effectiveness and 80 per cent coverage), prioritizing according to the number of interactions a person has cut deaths by 63.5 per cent compared to vaccination without any prioritization. A refinement of this strategy reduced fatalities by 71.7 per cent.

“The criteria for groups’ vaccination priority should not be those with the highest mortality but rather those the highest number of daily person-to-person interactions,” the authors wrote. Another advantage of focusing initially on younger people may be speed, which could be particularly important in vaccination programmes of the scale being envisaged.
Dr Bharat Pankhania, a senior clinical lecturer at the University of Exeter in the UK and consultant in communicable disease control, said that, from his experience in clinics, dealing with older people who are being vaccinated takes longer, potentially reducing throughput. “It takes time. In an emergency, if you can immunize as many people as you can, it’s a good idea,” he said.



![The Top & Most Popular Seafood Bucket Restaurants in Dubai for you [Never Miss]](https://uae24x7.com/wp-content/uploads/2020/09/8-seafood-in-a-bucket-scaled-e1600739237403.jpg)
![Procedures for Renewing the Driving License in Abu Dhabi [3 Simple Steps]](https://uae24x7.com/wp-content/uploads/2020/07/Capture-9-e1595666454466.jpg)





